Herpetic Sycosis Folliculitis
1. Presenting History
A 30-year-old female native of Sokoto, Western Nigeria, coming to the United States with fiancée for the first time presented to us one day after arrival at the hospital emergency room with a painful ulcerated lesion on her right ankle.
2. History Review
According to the patient, she noticed this lesion over the right ankle 10 days ago; she visited her pharmacist and there was a questionable history of trauma. The pharmacist in Nigeria performed incision and drainage of the pus and removal of unhealthy tissue at the lesion and started her on Trypsin, Amoxicillin/Clavulanate, and unknown pain medication. The pain from right ankle persisted and she went to community hospital and was treated with wound cleaning and other antibiotics. Patient then noticed bullous lesions over face and enlarging mouth ulceration.
3. Review of Systems
The patient was positive for fever, mouth ulcers, and stress and negative for weakness in any limbs, cough, eye pain, blurry vision, and history of keloid.
4. Past Medical History
The past medical history was significant for sickle cell trait.
5. Family History
The family history was noncontributory.
6. Personal History
Patient lives with her fiancé and has never been pregnant. She is a nonsmoker and denies alcohol or illicit substance use. Vaccinations status is not clear. Patient had no known history of BCG vaccination.
7. Physical Examination
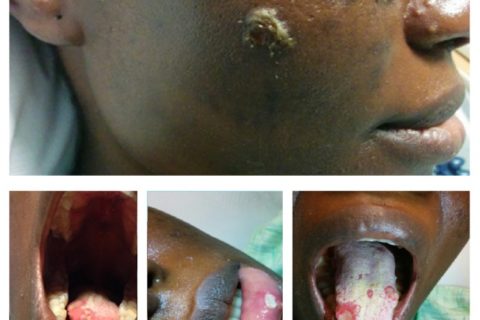
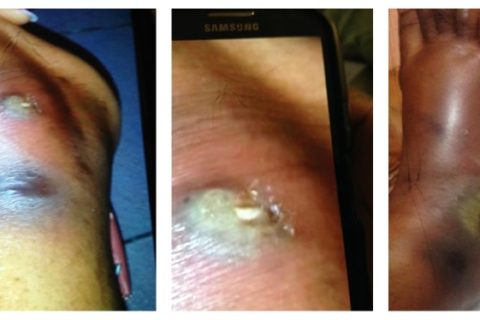
She is an African female. She was pleasant and in no distress. She had fever of 39.1°C, regular pulse of 73, BP of 121/74, and saturating 100% on room air. HEENT showed dry oral mucosa, multiple sized ulcerated lesions over tongue and palate and inner aspect of lower lip (Figure 2); no lymphadenopathy was found in neck, and the eye exam was normal. Lung and cardiovascular examinations were normal. Abdomen and genital exam was normal. Neuroexam was normal. Skin exam on the face showed multiple pustules, some with crusts and ulceration on elevated base measuring from 2 mm to 10 mm (Figure 1). One pustule measured 6 mm over the lateral aspect of the right leg. Ulcerated lesion was found over the right lateral malleolus measuring 3 cm × 4 cm with surrounding erythema and edema (Figure 3), and pulses were intact.

8. Investigations
CBC and BMP were within normal limits; ESR was elevated at 98 (normal rage 0–29 in females). HIV test was negative. X-ray of the ankle showed no bony abnormalities but a large soft tissue defect overlying the lateral malleolus with soft tissue swelling extending extensively along the dorsum of the foot. CT scan of the lower extremity and ankle showed no abscess or osteomyelitis. TB quantiferon was read as indeterminate high. Debrided tissue from the wound was tested with AFB stain. The acid-fast Bacilli (AFB) test was negative on the stain and culture. PCR was negative for M. Ulcerans. HSV IgM was elevated at 1 : 16 (normal; nonreactive); RPR was negative; ANA was negative; malaria screen was negative; and blood cultures were negative for bacteria, fungus, and virus
9. Initial Admission Diagnosis and Hospital Course
The initial admission diagnosis of the patient was cellulitis. Infectious disease consultant was called in to help in the management as the history was not clear on the day of presentation to the hospital.
She was started on broad spectrum antibiotics in the ER (Vancomycin and Zosyn). She had the surgical debridement of the wound in the leg. After surgery, topical enzymatic debridement was done with Santyl to her foot wound and wound vac was applied. Colchicine was started for the possibility of Behcet’s syndrome but was stopped after one day when the patient’s symptoms did not improve and pathology tests were negative. Dermatology recommended Valtrex for oral lesions. Patient’s face and oral lesions began to resolve after the first dose. Vancomycin was discontinued due to high levels which started affecting the renal function. All cultures were negative and antibiotics were discontinued. Wound vacuum was removed from right ankle before discharge from the hospital. Patient followed up in the ambulatory clinic and wounds have healed very well.
Original Source
Authors
Orange Park Medical Center Family Medicine GME, 2021 Professional Center Drive, Suite 100, Orange Park, FL 32073, USA
*Naganna Channaveeraiah: moc.liamtoh@sgcn
Academic Editor: Larry M. Bush
References
1. Ustaine R. P., Tinitigan R. Nongenital herpes simplex virus. American Family Physician. 2010;82(9):1075–1082. [PubMed] [Google Scholar]2. Thomas B. S., Bailey T. C., Bhatnagar J., et al. Mycobacterium ulcerans infection imported from Australia to Missouri, USA, 2012. Emerging Infectious Diseases. 2014;20(11):1876–1879. doi: 10.3201/eid2011.131534. [PMC free article] [PubMed] [CrossRef] [Google Scholar]3. Johnson P. D., Stinear T. P., Hayman J. A. Mycobacterium ulcerans-a mini-review. Journal of Medical Microbiology. Monash Medical Centre. 1999;48(6):511–513. [PubMed] [Google Scholar]4. Chi A. C., Neville B. W., Krayer J. W., Gonsalves W. C. Oral manifestations of systemic disease. American Family Physician. 2010;82(11):1381–1388. [PubMed] [Google Scholar]5. Mulryan C. Syphilis: recognizing the ‘great Pretender’ Practice Nursing. 2013;24(5) doi: 10.12968/pnur.2013.24.5.217. [CrossRef] [Google Scholar]6. Maccallum P., Tolhurst J. C., Buckle G., Sissons H. A. A new mycobacterial infection in man. The Journal of Pathology and Bacteriology. 1948;60(1):93–122. doi: 10.1002/path.1700600111. [PubMed] [CrossRef] [Google Scholar]7. Marion E., Carolan K., Adeye A., Kempf M., Chauty A., Marsollier L. Buruli ulcer in South Western Nigeria: a retrospective cohort study of patients treated in Benin. PLoS Neglected Tropical Diseases. 2015;9(1) doi: 10.1371/journal.pntd.0003443.e3443 [PMC free article] [PubMed] [CrossRef] [Google Scholar]