Tissue Necrosis due to Chloroform
Abstract
For many years, gutta-percha has been the root canal filling material of choice. Chloroform is one of the most efficient solvents widely used for gutta-percha removal in retreatment cases, despite being toxic and carcinogenic. The present case report discusses a chloroform extrusion through an existing perforation to the surrounding periodontal ligament space and subsequent necrosis in supporting bone and tissues, during an endodontic retreatment visit for an addicted patient. Subsequently, the management and preventive options are reviewed.
Key Words: Chloroform, Extrusion, Tissue Necrosis, Retreatment
Case Report
A 46 year old man with the history of drug abuse for the last 15 years without any systemic disease was referred to our office by a general practitioner. The dentist stated that he was doing a root canal treatment (RCT) for upper central and lateral incisors and canine without being aware of the occurrence of a perforation during access cavity preparation on lateral teeth. He prepared and obturated the canals. After providing the final radiography he decided to extirpate the GP from PDL space without anesthesia, by means of Chloroform, again being unaware of its leakage through the perforation site. The patient did not feel any pain neither unpleasant feeling which was believed to be due to his addiction. He was dismissed and the following morning he came up with a large missing zone in his buccal gingiva. He was immediately referred by his dentist to an endodontist for problem solving.
A large necrotic area in the gingival areas surrounding upper lateral incisor was obvious during clinical examination (Figures 1A and 1B). Lateral incisor had a large longitudinal perforation on mesial wall of the root. The patient reported history of drug abuse and that he had felt no pain or irritation during the retreatment. He also reported that he has experienced a medical surgery without anesthesia years before. After consulting with a periodontist, nonsurgical retreatment of upper central incisor and canine was performed by the endodontist (Figures 1C and 1D). Before treatment, the patient was referred for Cone Beam Computed Tomography (CBCT) for more evaluation that showed a long perforation on coronal half of mesial wall of maxillary left lateral incisor (Figure 1E).
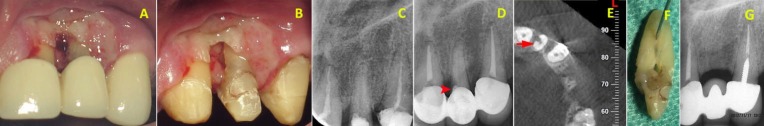
Tissue necrosis on maxillary left lateral incisor after two A) and ten B) days of injury; C) initial x-ray of the maxillary left lateral incisor; D) post-endodontic x-ray shows lateral perforation (red arrow head), along the mesial wall of the root in the lateral incisor; E) the CBCT shows the perforation in the mesial wall (red arrow); F) the gross view of perforation in the extracted tooth and; G) six-month follow-up
The lateral incisor was extracted and during a flap surgery the area was re-contoured. The extracted tooth showed a longitudinal perforation (Figure 1F). After the time needed for gingival healing, the patient treatment was completed with fixed partial denture between central incisor and the canine. Figure 1G shows the six-month follow-up.
Authors
aDepartment of Endodontics, Dental Branch, Islamic Azad University, Tehran, Iran;bDental Research Center, Research Institute of Dental Sciences, Shahid Beheshti University of Medical Sciences, Tehran, Iran*Corresponding author: Ladan Baradaran Mohajeri, No 4, 10th Neyestan, Pasdaran Ave., Tehran 19468 Iran. Tel: +98-21 88083591, Fax: +98-21 22763437, Email: ladanmohajeri@gmail.com
Copyright © 2013, Iranian Endodontic Journal.
References
1. Ribeiro DA. Do endodontic compounds induce genetic damage? A comprehensive review. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008;105(2):251–6. [PubMed] [Google Scholar]2. Abbasipour F, Akheshteh V, Rastqar A, Khalilkhani H, Asgari S, Janahmadi M. Comparing the effects of mineral trioxide aggregate and calcium enriched mixture on neuronal cells using an electrophysiological approach. Iran Endod J. 2012;7(2):79–87. [PMC free article] [PubMed] [Google Scholar]3. Barbosa SV, Burkard DH, Spangberg LS. Cytotoxic effects of gutta-percha solvents. J Endod. 1994;20(1):6–8. [PubMed] [Google Scholar]4. Vajrabhaya LO, Suwannawong SK, Kamolroongwarakul R, Pewklieng L. Cytotoxicity evaluation of gutta-percha solvents: Chloroform and GP-Solvent (limonene) Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2004;98(6):756–9. [PubMed] [Google Scholar]5. Edgar SW, Marshall JG, Baumgartner JC. The antimicrobial effect of chloroform on Enterococcus faecalis after gutta-percha removal. J Endod. 2006;32(12):1185–7. [PubMed] [Google Scholar]6. Ribeiro DA, Matsumoto MA, Marques ME, Salvadori DM. Biocompatibility of gutta-percha solvents using in vitro mammalian test-system. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;103(5):e106–9. [PubMed] [Google Scholar]7. Asgary S, Ahmadyar M. One-visit RCT of maxillary incisors with extensive inflammatory root resorption and periradicular lesions: A case report. Iran Endod J. 2011;6(2):95–8. [PMC free article] [PubMed] [Google Scholar]8. Ribeiro DA, Marques ME, Salvador DM. In vitro cytotoxic and non-genotoxic effects of gutta-percha solvents on mouse lymphoma cells by single cell gel (comet) assay. Braz Dent J. 2006;17(3):228–32. [PubMed] [Google Scholar]9. Huang X, Ling J, Wei X, Gu L. Quantitative evaluation of debris extruded apically by using ProTaper Universal Tulsa rotary system in endodontic retreatment. J Endod. 2007;33(9):1102–5. [PubMed] [Google Scholar]10. Metzger Z, Ben-Amar A. Removal of overextended gutta-percha root canal fillings in endodontic failure cases. J Endod. 1995;21(5):287–8. [PubMed] [Google Scholar]11. Martos J, Bassotto AP, Gonzalez-Rodriguez MP, Ferrer-Luque CM. Dissolving efficacy of eucalyptus and orange oil, xylol and chloroform solvents on different root canal sealers. Int Endod J. 2011;44(11):1024–8. [PubMed] [Google Scholar]12. Mushtaq M, Masoodi A, Farooq R, Yaqoob Khan F. The dissolving ability of different organic solvents on three different root canal sealers: in vitro study. Iran Endod J. 2012;7(4):198–202. [PMC free article] [PubMed] [Google Scholar]