Abdominal wall disruption with evisceration after blunt trauma
Case presentation
A 65-year-old man was lying under the cargo bed of a lorry, inspecting the undercarriage. Unaware of this, the lorry driver started his journey and the rear wheel rolled over the patient’s lower abdomen and pelvis.
Bystanders who witnessed the accident transported him to the nearest hospital within 30 min of sustaining injury. Apart from covering the abdominal wound with an article of clothing, no prehospital resuscitative measures were instituted.
Despite being haemodynamically stable, this patient was markedly distressed due to pain. There was a large laceration approximately 20 cm in length at the left side of the abdomen from which small and large bowel eviscerated and a superficial paramedian laceration in the upper left abdomen (figure 1). A healed upper midline scar was also present after exploratory laparotomy for perforated peptic ulcer disease more than 10 years prior to this presentation.
Resuscitation was started by securing intravenous access and infusing isotonic crystalloids. We administered opioid analgesia, proton pump inhibitors and broad-spectrum antibiotics (metronidazole and ceftriaxone) in the emergency room. The exposed viscera were washed with 1 L of normal saline and then wrapped in a moist towel.
This patient met an indication for exploratory laparotomy to reduce the viscera, repair the abdominal wound and address any additional injuries encountered. However, since he was stable, we opted to take him to the radiology department first to exclude orthopaedic injuries that may have required operative intervention.
Treatment
Under general anaesthesia, the abdominal laceration was extended medially to enter the abdomen. A thorough inspection of the intra-abdominal viscera and retroperitoneum was performed. The eviscerated bowel was viable but there were two small areas of perforation (rupture) at the jejunum. The bowel edges were debrided and primarily repaired. There were no additional intra-abdominal injuries noted. The viscera were lavaged with 3 L of normal saline and reduced into the abdomen. The abdomen was then closed in layers. No drains were used in this case.
Outcome and follow-up
The patient was discharged to the high dependency unit for continued care. The postoperative period was complicated by a prolonged ileus but this resolved on day 7 with bowel rest, nasogastric drainage and infusions of maintenance intravenous fluid and electrolytes. Thereafter, there was an uneventful recovery, with no signs of intra-abdominal collections. The patient was eventually discharged from hospital 12 days after admission.
One year postinjury, there was complete healing of the abdominal wounds (figure 3) without evidence of an incisional hernia. The iliac and acetabular fractures have united, although there is a pincher deformity of the acetabular rim remaining (figure 4).
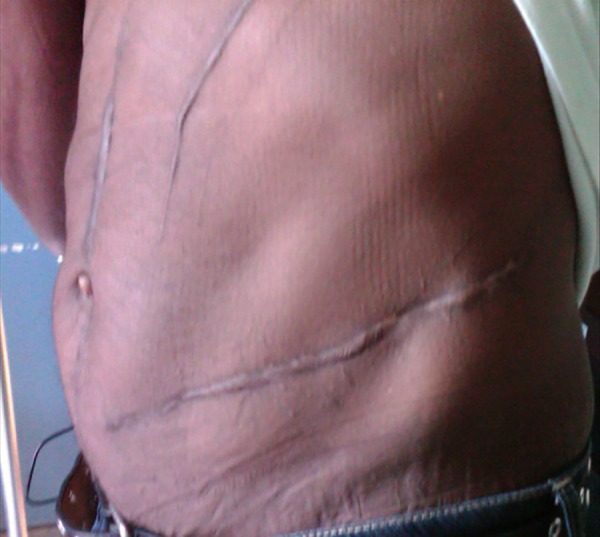
Surface of the abdomen 1-year post-injury. There is complete healing without evidence of an incisional hernia.
