Faucial Diphtheria
Case Report
A 12-year-old Muslim male complained of low-grade fever and gradually progressive sore throat, along with dysphagia and gradually increasing swelling in the neck, leading to “bull-neck” formation for the last 10 days. He had an incomplete vaccination status, as he did not receive a DT booster at 5 years. On clinical examination, he had bilateral tonsillar enlargement with formation of a grayish-white membrane involving the tonsils, posterior pharyngeal wall and soft palate. His pulse rate was 110/min, and BP was 130/90 mmHg. He was unable to deglut . No skin lesions were found. No significant past medical or surgical history. No contact or family history could be traced.
Investigations
A routine hemogram revealed neutrophilic leukocytosis, high ESR, mild hypochromic microcytic anemia and mild thrombocytosis.
X-ray and CT-scan of neck revealed bilateral tonsillar enlargement, along with peritonsillar and peri-pharyngeal collection.
Sputum and pus for Z-N stain were negative for AFB. Monteux tuberculin test was negative. Throat swab for KLB was positive.
ECG showed sinus tachycardia along with ST/T wave changes in all precordial and chest leads.
Differential Diagnosis
- Faucial diphtheria
- Tonsillar abscess
- Tuberculosis
- Faucial neoplasm
- Diphtheria myocarditis
- Viral infection
- Infection(s) in a case of congenital heart disease
TREATMENT
We administered 100,000 units of ADS IM and started IV crystalline penicillin, but his condition remained the same for the next 2 days; not able to drink anything.
From day 3, his fever regressed, neck swelling started regressing, and in the morning, he coughed out the membrane. His throat now became much clearer, and he continued a povidone-iodine solution gargle as advised, but over-all signs of well-being were not there.
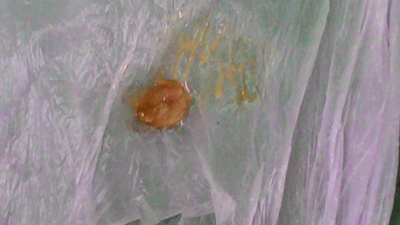
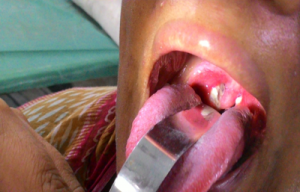
He received antibiotics for 10 days more, and then his condition started improving. But, in the meantime, he developed features of heart failure and abnormal ECG findings on day 13, which was managed with fluid restriction, ACE inhibitors, low-dose diuretics and Carvedilol.
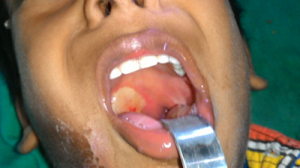
Outcome and Follow Up
After 10 days, the patient was hemodynamically stable and was discharged. The patient is being followed up in the out-patient department and is doing well, 4 months after the attack.
Original source
Authors
Dr. Swapan Samanta and Dr. Malay Acharyya
