Isolated trochlear nerve palsy with midbrain hemorrhage
Summarized by: Granit Rudi, MD
Source: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2841378/
Copyright © Indian Journal of Ophthalmology. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
The term “palsy” refers to partial loss of a nerve’s function. The Trochlear nerve, a small nerve part of the 12 nerves that originate inside the head (called “cranium in latin, hence why they’re called “cranial nerves”) innervates solely one muscle of the eye, the superior oblique muscle. The superior oblique muscle helps to keep the eyes aligned, so if there’s a loss of it’s nerve supply (the Trochlear nerve in this case), the patient will get a misalignment of his/her eyes. The medical term of misalignment of the eyes is called “strabismus”. This partial loss of the trochlear nerve’s function can have many causes, but in most cases the patients who have it are born with it (congenital palsy), but there are also other causes such as direct trauma to the nerve, or high blood pressure rupturing the small blood vessels that supply the nerve with blood. Other causes such as brain tumors or brain hemorrhages very rarely give trochlear nerve palsy as a sole symptom, because they usually cause other problems as well, such as severe headaches or loss of consciousness.
That’s why this case report by Raghavendra S. et al is very interesting. It reports an 18 year old patient who suffered brain hemorrhage due to a congenital malformation of the blood vessels (called “cavernoma”) rupturing spontaneously. After presenting with double-vision (diplopia), the standard eye examinations revealed a misalignment of the eyes consistent with trochlear nerve palsy. After not being able to reach a clear diagnosis, the doctors ordered a deep brain scan with magnetic resonance imaging. As rarely reported, they found that the patient had actually suffered brain hemorrhage, with images showing lesions near the mid-brain. After adequate treatment, the patient’s double vision was alleviated. At six months follow-up, the lesion in the brain had also remained static and the patient didn’t report any neurological deficits.
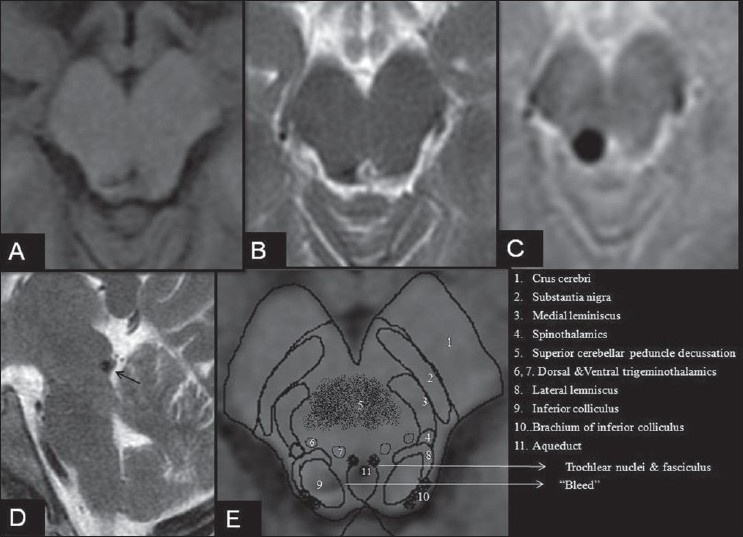
MRI brain in a patient with isolated acute left trochlear nerve palsy. Axial T1 SE (A), axial T2 FSE (B), Axial T2*GRE (C) and Sagittal T2WI(D) showing a hypointense lesion in the right tectal region at the level of the inferior colliculus with intense blooming on gradient imaging without any flow voids. E, schematic representation of the anatomical structures of the midbrain at the level of the inferior colliculus overlapped on Figure A. Note: Increased hypointensity of a paramagnetic substance such as blood on T2*GRE (gradient) imaging is termed as blooming