Successful Facial Reconstruction in Complex Facial Avulsion Injury
A 56 years old female presented with history of road traffic accident with resultant avulsion of her left side of face. There was degloving and avulsion of the left hemi-face including the upper lip nose, forehead skin and eyebrow, upper and lower eyelids and the entire left cheek. The zygomatic bone was also avulsed and displaced laterally. The globe was displaced inferiorly towards the maxillary sinus
The patient was immediately resuscitated airway management, control of bleeding and maintainence of circulation. Other injuries were quickly ruled out and CT scan with 3D CT of the face was done. CT scan showed avulsion of the zygoma with lateral blowout fracture of the orbit. There was no brain injury. The vision was tested for finger counting which was present at 2 to 3 feet. Decision was taken for an immediate single stage reconstruction of the bony as well as soft tissue avulsion.
The patient was taken for surgery and under anesthesia the wound was thoroughly washed with normal saline and diluted betadine solution. All contaminants and foreign bodies were removed. Careful debridement was done and crushed nonviable tissues were excised. The orbital cavity was then reconstructed. The globe was seen to be displaced towards the maxillary sinus. The avulsed zygoma still had soft tissue attachments. There was a piece of lateral orbital rim with the soft tissue flap which was repositioned and the lateral orbital wall was reformed. The fractures were fixed with titanium miniplates. The eyeball was thus repositioned to its original position and the volume of the orbital cavity was restored (Figure 2 and and 3).
Once the bony fixation was done the soft tissue reconstruction was started. The degloved flap was repositioned. Tacking sutures were taken to the periosteum wherever possible to keep the flap in place. The upper lip was repaired in layers after marking the anatomical landmarks. The mucosa and muscle were repaired with absorbable sutures and skin with nylon. The nose was reconstructed with repair of the mucosal lining followed by repair of the cartilage framework. The nasal ala was repositioned and the skin was repaired. The eyelids and forehead were repaired in layers (Figure 4). The post-operative course was uneventful. The patient had no problems in visual acuity. The patient was on higher antibiotics for five days and discharged. The sutures were removed on 7th postoperative day. All wounds healed well without any flap necrosis (Figure 5). The patient had normal vision and full facial functions at six months follow up.
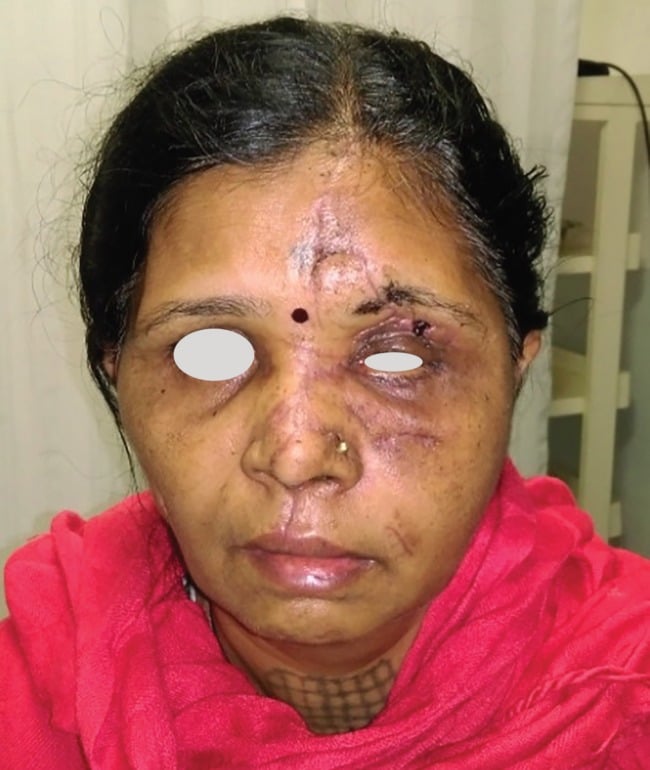
Postoperative results after 1 month



