Surgical correction of residual facial deformity following conservative excision of a giant maxillary ossifying fibroma
Zhuoxia Wu, MD,a Yunlong Xing, MD,a Xin Liu, PhD,b Wanying Chen, MD,a Jiao Kong, MD,a Ronghui Wu, MD,a and Lianbo Zhang, PhDa,∗
2. Case report
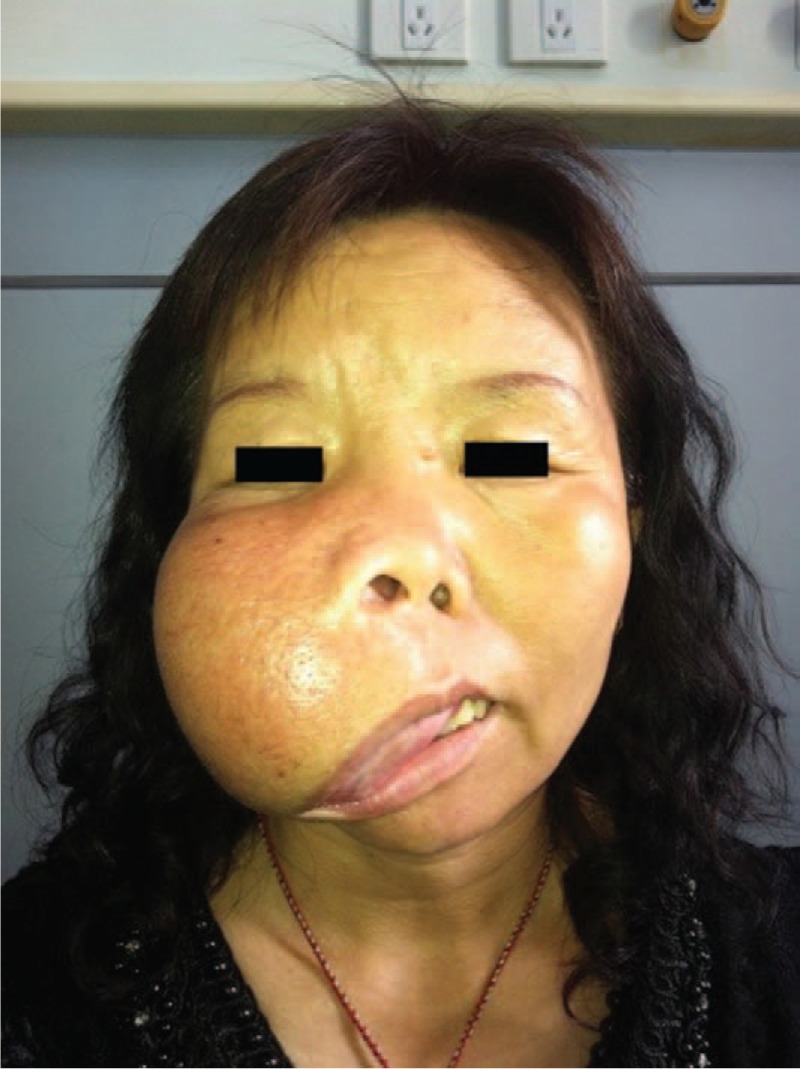
A 44-year-old female patient presented to our department in November 2013 with a chief complaint of a giant swelling on the right side of her face that had gradually increased in size over 30 years. She experienced no related pain, paresthesia, or tenderness. On examination, the swelling in the right maxillary region measured 15 × 15 × 10 cm in size and had normal skin appearance. Additional findings included apparent drooping of the upper lip with a widened philtrum, distorted appearance of the nose and external nares, disappearance of the right alar groove, exposed right palate, and partially exposed teeth on the right side. There was no associated temperature or color change and no tenderness, but the skin surface was thickened. Inside the oral cavity, the maxillary lesion occluded the right buccal and labial vestibules, and the right buccal vestibule and palate were expanded with a normal mouth opening and shifted maxillary teeth with redundant oral mucosa (Figs.1 and 2).
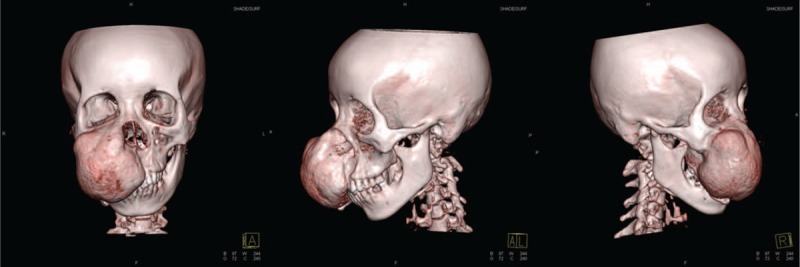
Computed tomography scan and 3-dimensional reconstruction revealed a 13 × 13 × 9 cm expansile lesion arising from the right maxilla with defined anterior margin and rough surface. Superiorly, the lesion was eroding the right inferior orbital wall and posterosuperiorly, the lesion had displaced the maxillary sinus, which appeared shrunken. The lesion involved the right os nasal medially and the right alveolar bone distally, and appeared as a solitary radiolucent cyst-like mass with irregular radiodensity. The cortex and medulla were not clearly separated (Figs.3 and 4).
Because of the size of the maxillary tumor, reconstruction was necessary after complete resection to maintain the function of adjacent organs that had been invaded by the tumor. However, the patient refused bone or metal grafting for financial reasons and was treated with conservative excision after exposing the tumor using the Weber–Fergusson approach. We removed as much tumor tissue as possible while maintaining functional bone tissue and excised the excess skin and oral mucosa (Fig. 5). Histopathologically, the lesion appeared as trabecular bone surrounded by osteoblasts scattered within proliferative fibrous tissue. Trabecular bone was thickened and arranged in parallel sheets with surrounding calcification, which confirmed the diagnosis of OF (Fig. 6).
Two years postoperatively, in November 2015, the patient complained of conspicuous scars and drooping of the upper lip on the right side with no visible tumor swelling (Fig. 7). To improve her facial appearance, we performed a second surgery using the same approach to excise scar tissue and partial residual tumor, correcting the droop in the right upper lip. During recovery, local infection caused by bone wax rejection leads to subcutaneous adhesion of the right lower eyelid, which finally resulted in right lower eyelid ectropion through scar contracture (Fig.8). In February 2017, with no obvious increase in volume of the tumor, the patient underwent corrective surgery for the valgus deformity in the right lower eyelid. We separated the subcutaneous tissue to relax the constricted scar and implanted a crescent-shaped silicone prosthesis to avoid recurrence of subcutaneous adhesions and scar contracture (Fig. 9). Following this third surgery in January 2018, the ectropion deformity in the right lower eyelid improved dramatically and no obvious swelling of tumor was found (Fig. 10); however, the patient was still followed for complications and tumor recurrence regularly.
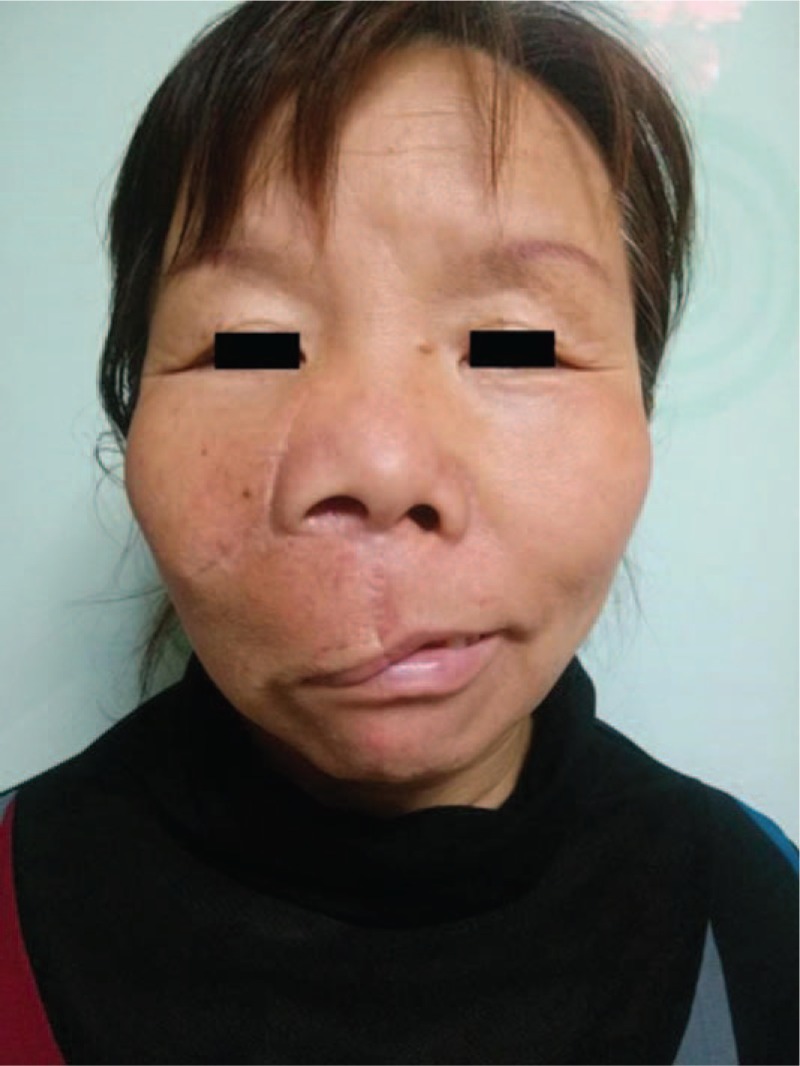
Two years after the primary excision, the patient complained of conspicuous scars and drooping of the upper lip on the right side with no visible increase in volume of the tumor.

Fifteen months after the second surgery, local infection caused by bone wax rejection leads to subcutaneous adhesion of the right lower eyelid, which finally resulted in right lower eyelid ectropion through scar contracture.
Author contributions
Data curation: Wanying Chen.
Investigation: Jiao Kong.
Resources: Yunlong Xing, Xin Liu, Ronghui Wu.
Supervision: Lianbo Zhang.
Validation: Lianbo Zhang.
Writing – original draft: Zhuoxia Wu.
Writing – review & editing: Zhuoxia Wu.
References
[1] Waldron CA. Fibro-osseous lesions of the jaws. J Oral Maxillofac Surg 1993;51:828–35. [PubMed] [Google Scholar]
[2] Brademann G, Werner JA, Janig U, et al. Cemento-ossifying of the premastoid region: case report and review of the literature. J Larygol Otol 1997;111:152–5. [PubMed] [Google Scholar]
[3] Magu S, Airon RK, Mishra DS, et al. Images: cementoossifying fibroma of the maxilla. Indian J Radiol Imaging 2000;10:103–4. [Google Scholar]
[4] Chang CC, Hung HY, Chang JY, et al. Central ossifying fibroma: a clinicopathologic study of 28 cases. J Formos Med Assoc 2008;107:288–94. [PubMed] [Google Scholar]
[5] Eversole LR, Leider AS, Nelson K. Ossifying fibroma: a clinicopathologic study of sixty-four cases. Oral Surg Oral Med Oral Pathol 1985;60:505–11. [PubMed] [Google Scholar]
[6] Martín-Granizo R, Sánchez-Cuellar A, Falahat F. Cemento ossifying fibroma of the upper gingivae. Otolaryngol Head Neck Surg 2000;122:775. [PubMed] [Google Scholar]
[7] Silveira DTD, Cardoso FO, Silva BJAE, et al. Ossifying fibroma: report on a clinical case, with the imaging and histopathological diagnosis made and treatment administered. Rev Bras Ortop 2016;51:100–4. [PMC free article] [PubMed] [Google Scholar]
[8] Shafer WG, Hine M, Levy BM. A Text Book of Oral Pathology. 4th ed.Philadelphia, PA: WB Saunders; 1983. [Google Scholar]
[9] Mintz S, Velez I. Central ossifying fibroma: an analysis of 20 cases and review of the literature. Quintessence Int 2007;38:221–7. [PubMed] [Google Scholar]
[10] Canger EM, Celenk P, Kayipmaz S, et al. Familial ossifying fibromas: report of two cases. J Oral Sci 2004;46:61–4. [PubMed] [Google Scholar]
[11] Saiz-Pardo-Pinos AJ, Olmedo-Gaya MV, Prados-Sánchez E, et al. Juvenile ossifying fibroma: a case study. Med Oral Patol Oral Cir Bucal 2004;9:456–8. [PubMed] [Google Scholar]
[12] Tchane IB, Adjibabi W, Biaou O, et al. Cemento-ossifing fibroma: two cases. Rev Stomatol Chir Maxillofac 2005;106:30–2. [PubMed] [Google Scholar]
[13] Koury ME, Regezi JA, Perrott DH, et al. Atypical fibro-osseous lesions: diagnostic challenges & treatment concepts. Int J Oral Maxillofac Surg 1995;24:162–9. [PubMed] [Google Scholar]
[14] Jurlina M, Skitarelić N, Passali D, et al. Endonasal endoscopic resection of ossifying fibroma involving the ethmoid sinus, orbit and anterior skull base: case report and literature review. Acta Otorhinolaryngol Italica 2016;36:144–8. [PMC free article] [PubMed] [Google Scholar]
[15] Figueiredo LM, de Oliveira TF, Paraguassú GM, et al. Psammomatoid juvenile ossifying fibroma: case study and a review. Oral Maxillofac Surg 2014;18:87–93. [PubMed] [Google Scholar]
[16] Titinchi F, Morkel J. Ossifying fibroma: analysis of treatment methods and recurrence patterns. J Oral Maxillofac Surg 2016;74:2409–19. [PubMed] [Google Scholar]
[17] Ram H, Mohammad S, Husain N, et al. Huge ossifying fibroma of the maxilla. J Maxillofac Oral Surg 2014;13:337–40. [PMC free article] [PubMed] [Google Scholar]
[18] Brannon RB, Fowler CB. Benign fibro-osseous lesions: a review of current concepts. Adv Anat Pathol 2001;8:126–43. [PubMed] [Google Scholar]
[19] Charles AW. Neville BW, Damm DD, Allen CM, et al. Doenças do osso. Oral and Maxillofacial Pathology 2nd ed.Philadelphia, PA: WB Saunders; 2002. 511–53. [Google Scholar]
[20] Gurol M, Uckan S, Guler N, et al. Surgical and reconstructive treatment of a large ossifying fibroma of the mandible in a retrognathic patient. J Oral Maxillofac Surg 2001;59:1097–100. [PubMed] [Google Scholar]
[21] Tyagi A, Chaudhary S, Gupta V. Ipsilateral maxillo-mandibular ossifying fibroma. J Maxillofac Oral Surg 2015;14:1–6. [PMC free article] [PubMed] [Google Scholar]
[22] Williams HK, Mangham C, Speight PM. Juvenile ossifying fibroma: an analysis of eight cases and a comparison with other fibro-osseous lesions. J Oral Pathol Med 2000;29:13–8. [PubMed] [Google Scholar]
[23] Ranganath K, Kamath SM, Munoyath SK, et al. Juvenile psammomatoid ossifying fibroma of maxillary sinus: case report with review of literature. J Maxillofac Oral Surg 2014;13:109–14. [PMC free article] [PubMed] [Google Scholar]
[24] Agarwal SP, Kumar S, Singh HP, et al. Huge ossifying fibroma maxilla. Natl J Maxillofac Surg 2015;6:241–3. [PMC free article] [PubMed] [Google Scholar]
Copyright
Copyright © 2018 the Author(s). Published by Wolters Kluwer Health, Inc.This is an open access article distributed under the terms of the Creative Commons Attribution-Non Commercial-No Derivatives License 4.0 (CCBY-NC-ND), where it is permissible to download and share the work provided it is properly cited. The work cannot be changed in any way or used commercially without permission from the journal. http://creativecommons.org/licenses/by-nc-nd/4.0