A Case of Aplasia Cutis Congenita Type VI: Bart Syndrome
Yasmin Alfayez, Sahar Alsharif,* and Adel Santli
Case Report
A 4-h-old male newborn presented with complete absence of skin over the anteromedial aspect of both lower legs since birth. The baby was born to a 23-year-old primigravida mother via normal vaginal delivery. Both pregnancy and delivery were uncomplicated. The mother denied any history of exposure to medications or radiation during her pregnancy. The parents were not relatives. There was no family history of similar conditions or any skin diseases.
The baby’s Apgar scores were normal, but he was admitted to the neonatal intensive care unit due to this skin lesion. Otherwise, the baby seemed to be in a good health. He had normal weight, length, head circumference, and vital signs. On physical examination, there were symmetrical bilateral absences of skin over the anteromedial aspect of the legs, starting from the knees and extending to the dorsal and medial plantar aspect of the feet. The lesions had sharply demarcated borders covered by a red ultrathin translucent membrane, and vascular structures were easily visualized (Fig. 1). Some nails of the fingers and toes were dystrophic. The scalp and the mucous membranes were not affected. Systemic examination was normal. After 5 days, the baby developed blisters over the preexisting lesions. Blistering also appeared over normal skin in response to minor trauma or friction.
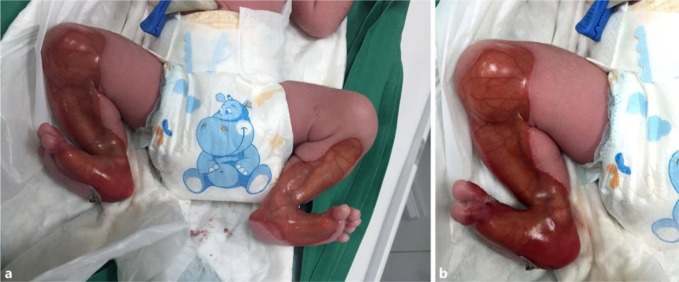
a, b Symmetrical bilateral absence of skin over the anteromedial aspect of the legs, starting from the knees and extending to the dorsal and medial plantar aspects of the feet. The lesions have sharply demarcated borders covered by a red ultrathin translucent membrane, and vascular structures were easily visualized.
Several laboratory investigations were performed; the baby’s complete blood count, electrolytes, as well as liver and renal function tests were within normal limits, and serologic tests for infection were negative. Ophthalmological examination, abdominal and cranial ultrasound screening, and echocardiography revealed normal findings.
A skin biopsy was taken from a fresh blister over the thigh. Histopathological study of the skin biopsy showed subepidermal blister formation, which was consistent with epidermolysis bullosa. Immunofluorescence staining and electron microscopy were not available in our hospital. The combination of congenital localized absence of skin over the lower extremities, epidermolysis bullosa, and nail abnormalities led to the diagnosis of aplasia cutis congenita (ACC) type VI (Bart syndrome).
We performed conservative wound care with topical antibacterial cream (fusidic acid cream 2%) applied twice per day and nonadhesive dressing. After 1 week, the infant was discharged, and the mother was given detailed instructions about handling the baby and continuing local wound care.
The patient returned for follow-up in the outpatient dermatology clinic every 2 weeks for 2 months. At the 2-month follow-up visit, the patient was in good health and was well fed on formula without any complications. There was no difficulty in urination or defecation. The previous lesion healed with scarring and milia formation (Fig. 4, Fig. 5).
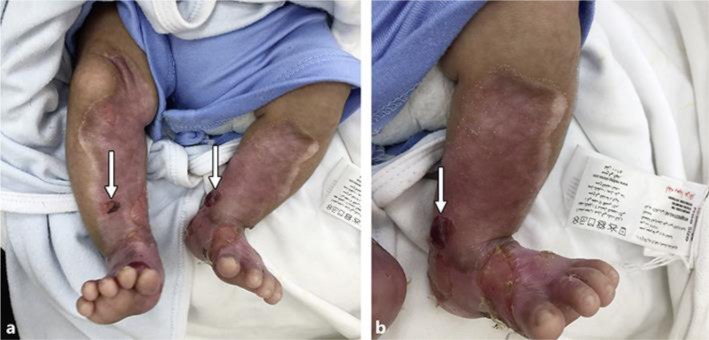
a, b After 2 months, the lesions were completely healed with hypopigmented scarring and milia formation. There were also some bullae, as shown by the arrows.
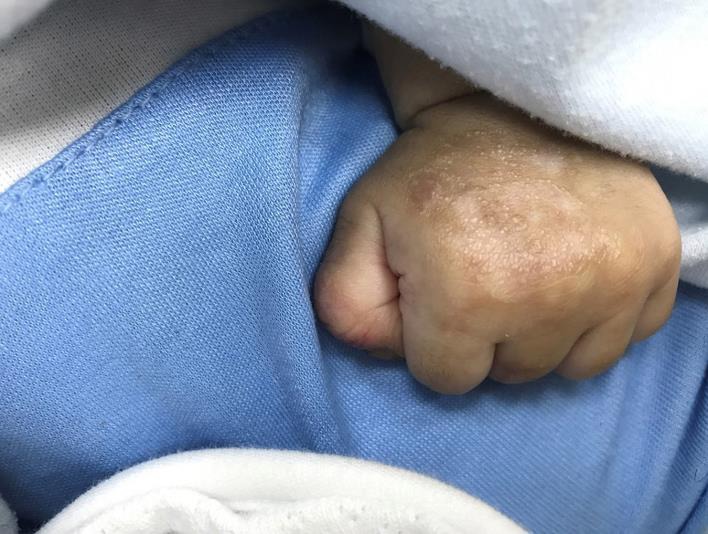
Milia formation.
References
References
- Rajpal A, Mishra R, Hajirnis K, Shah M, Nagpur N. Bart’s syndrome. Indian J Dermatol. 2008;53:88–90. [PMC free article] [PubMed] [Google Scholar]
- Bart BJ, Gorlin RJ, Anderson VE, Lynch FW. Congenital localized absence of skin and associated abnormalities resembling epidermolysis bullosa. A new syndrome. Arch Dermatol. 1966;93:296–304. [PubMed] [Google Scholar]
- Duran-McKinster C, Rivera-Franco A, Tamayo L, de la Luz Orozco-Covarrubias M, Ruiz-Maldonado R. Bart syndrome: the congenital localized absence of skin may follow the lines of Blaschko. Report of six cases. Pediatr Dermatol. 2000;17:179–182. [PubMed] [Google Scholar]
- Frieden IJ. Aplasia cutis congenita: a clinical review and proposal for classification. J Am Acad Dermatol. 1986;14:646–660. [PubMed] [Google Scholar]
- Casanova JM, Martí RM, Baradad M, Egido R, Mascaró JM. Bart syndrome associated to lethal junctional epidermolysis bullosa (Herlitz form) (in Spanish). Actas Dermosifiliogr. 2006;97:658–661. [PubMed] [Google Scholar]
- Kulalı F, Bas AY, Kale Y, Celik IH, Demirel N, Apaydın S. Type VI aplasia cutis congenita: Bart’s syndrome. Case Rep Dermatol Med. 2015;2015:549825. [PMC free article] [PubMed] [Google Scholar]
- Kothari C, Doshi N, Avila A, Martin D. Visual diagnosis: newborn with absence of skin. Pediatr Rev. 2014;35:e49–e52. [PubMed] [Google Scholar]
- Kuvat SV, Bozkurt M. Conservative treatment of a patient with epidermolysis bullosa presenting as Bart syndrome: a case report. Case Rep Med. 2010;2010:302345. [PMC free article] [PubMed] [Google Scholar]
Articles from Case Reports in Dermatology are provided here courtesy of Karger Publishers
Author Information
Dermatology Department, King Fahad Armed Force Hospital, Jeddah, Saudi Arabia*Sahar Alsharif, PO Box 16688, Makkah 21955 (Saudi Arabia), E-Mail
Copyright and License Information
Copyright © 2017 by S. Karger AG, BaselThis article is licensed under the Creative Commons Attribution-NonCommercial-4.0 International License (CC BY-NC) (http://www.karger.com/Services/OpenAccessLicense). Usage and distribution for commercial purposes requires written permission.