Anti-hypertension drug related Angioedema
- Ian Wisecarver, Sanjay Kamboj, MD, David Galambos, Michelle Korah-Sedgwick, MD, Ross McCarron, MD, Fred Lopez, MD
CASE PRESENTATION
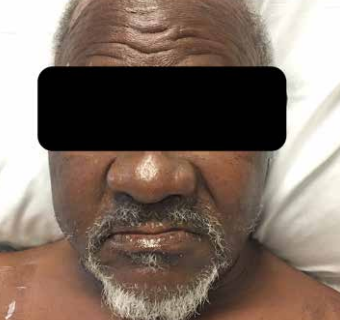
A 72 year-old African American man with a past medical history of hypertension, heart failure with reduced ejection fraction, and alcohol use presented to the emergency department (ED) with a chief complaint of a one day history of facial swelling (Figure 1).
On the day prior to presentation, the patient noted that he took a dose of a friend’s lisinopril in an attempt to relieve atraumatic left lower leg swelling. The swelling had been present for the past week and he believed it was caused by his previously diagnosed heart failure. Upon awakening the next morning, he noticed new onset lip swelling and took another tablet of lisinopril in an attempt to relieve the swelling. The swelling in his lips progressively worsened throughout the day, prompting him to seek medical attention at the hospital. On presentation to the hospital, the patient denied difficulty breathing, throat swelling, and any previous history of allergic reactions. The patient was afebrile, normotensive, tachycardic, his oxygen saturation was 99% on ambient air, and he was in no apparent distress. He had significant non-pitting, nonerythematous edema of both his upper and lower lips, left cheek, left periorbital area, and mild edema of the right periorbital area. He did not show any signs of lingual or posterior.
One and a half hours after admission, the edema continued to worsen and prompted concern regarding possible airway compromise due to evolving pharyngeal edema. The emergency medicine physician documented posterior pharyngeal wall edema (Figure 2) and recommended elective intubation to protect the patient’s airway. However, the patient elected to refuse intubation in hopes that the swelling would resolve shortly. While in the ED, a working diagnosis of ACEi-induced angioedema was established and the patient was treated with an immediate transfusion of two units of fresh frozen plasma (FFP). During this time, the hospital pharmacy was consulted about the availability of icatibant, a bradykinin B2-receptor antagonist used in the treatment of Hereditary Angiodema which has also been used off-label in management of ACEiinduced angioedema. To rule out hereditary angioedema and acquired angioedema, C1 inhibitor function and protein levels, C4 complement, and C1q levels were ordered. Results of all were within normal limits.
Two hours after his initial presentation to the ED, the patient was admitted to the Intensive Care Unit (ICU) due to concern for impending airway compromise secondary to worsening facial and pharyngeal swelling. Five hours after admission to the ICU, the patient was emergently intubated (Figure 4). On the day following his admission to the ICU, the patient’s angioedema continued to progress and he was given another two units of FFP. During this time, the patient began exhibiting symptoms of alcohol withdrawal, most notably tachycardia and hypertension. These symptoms were well-controlled with clonidine patches and diazepam injections
Approximately 36 hours after his initial presentation to the ED, the patient’s facial swelling began to subside. On hospital day three, his airway was deemed stable and the patient was extubated. The patient was discharged to home on day six of his hospital stay and was instructed to follow up in clinic as an outpatient for management of his hypertension and heart failure. The patient was instructed not to take any angiotensin converting enzyme inhibitor or angiotensin II receptor blocker class medications in the future and was told to return to the ED if any of his symptoms returned.


