Corneal injury secondary to silver nitrate stick mistaken for cotton bud
Corneal injury secondary to silver nitrate stick mistaken for cotton bud
Abstract
Purpose
This case report highlights the potential for error when removing corneal foreign bodies in a shared speciality area in Accident and Emergency (A&E).
Observations
This case presents the accidental use of a silver nitrate stick rather than a cotton bud to remove a corneal foreign body. This resulted in a corneal injury requiring ophthalmological referral and management with topical antibiotics, topical steroids and lubricants.
Conclusions
Mistaking a silver nitrate stick for a cotton bud is a tangible risk in a busy A&E and can result in significant corneal injury. Clinicians and departments can greatly reduce this risk by having separate and secure storage of similar consumables, as well as keeping consumables in original packaging and discarding of the remainder after a pack has been opened. Minimizing the risk for error will better safeguard and improve patient safety.
1. Introduction
Cotton buds are regularly used in an Accident and Emergency (A&E) setting for the removal of foreign bodies from the cornea. In many Emergency Departments in the areas where procedures are done, there is a wide array of different consumables used by different specialties that can have a very similar appearance but different functions. This is a cause for potential error. Misusing a silver nitrate stick rather than a cotton bud can cause significant corneal injury for example. Small measures with regards to separate and secure storage of these similar consumable, as well as removing all used consumables can greatly reduce this risk.
2. Case presentation: medical history, clinical features
A 15 year old boy attended A&E after being struck by a snowball to the left eye earlier the same day. On slit lamp examination, a corneal abrasion and corneal foreign bodies were noted. The A&E doctor at this point picked up what he thought to be a cotton bud in order to remove the foreign bodies. It was later realised that a silver nitrate stick had been inadvertently used in error. It had been brushed against the cornea three times before the error was realised.
The eye was immediately irrigated with water and the pH tested at 7. Further irrigation was completed with 400mls of normal saline 0.9% solution. The mistake was explained to the patient and full duty on candour was adhered to. Ophthalmological opinion was sought and the patient attended an emergency eye clinic the following morning. On assessment, he was diagnosed with a left corneal abrasion from the snowball injury and corneal opacity secondary to chemical injury due to the use of the silver nitrate stick.
3. Outcome, prognosis and follow up
The patient was treated with chloramphenicol 1% ointment four times a day for infection prophylaxis and lubrication to provide comfort, and cyclopentolate 1% eye drops three times a day to reduce ciliary spasm. However, on examination there were clinical features of keratolysis with a central corneal opacity and corneal thinning (Fig. 1). The area of thinning measured 4.0mm by 2.0mm in the widest dimensions with approximately 50% stromal thinning based on slit lamp examination. He had worsening visual acuity of only being able to count fingers. Therefore, he was commenced on topical steroids (dexamethasone 0.1% four times a day) to control the clinical appearing ocular surface inflammation on day five after initial presentation. Over a period of two months his vision improved back to baseline vision of 6/5 with minimal corneal stromal scarring off the visual axis. He tapered the use of topical steroids over a two month period and continues the use topical ocular lubricants as required for symptoms of dry eye.
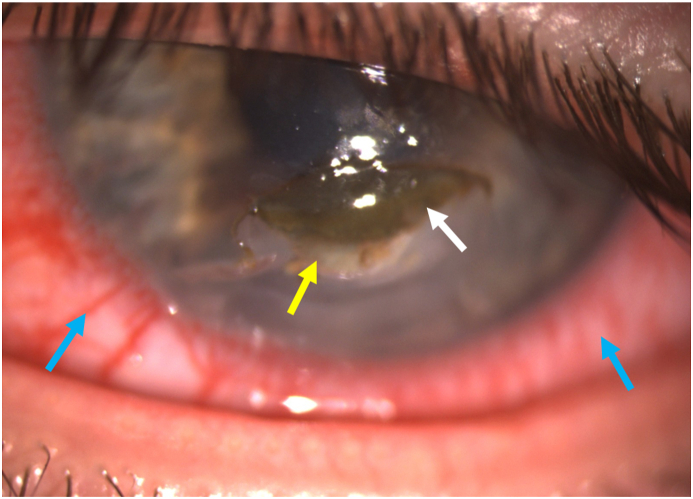
Photograph of corneal injury four days following presentation to A&E. There is corneal stromal thinning and opacity (yellow arrow) and adjacent necrotic corneal tissue (white arrow). There is also marked bulbar conjunctival injection (blue arrows). (For interpretation of the references to colour in this figure legend, the reader is referred to the Web version of this article.)
4. Discussion including review of similar published cases
This case illustrates the potential ease by which a silver nitrate stick can be mistaken for a cotton bud (Fig. 2). Application of a silver nitrate stick to the eye can cause significant corneal injury which has the potential to result in significant inflammation, corneal melting, corneal scarring and significant visual impairment.

Comparison of silver nitrate sticks (left) and cotton buds (right).
Considering the relatively common presentation of corneal foreign bodies, few comparable cases were found on literature search. “Severe silver nitrate injury to the eye” was documented by Grayson et al. in a case report in 1970.1 The report describes silver nitrate being used to cauterise a wound following removal of an upper eyelid chalazion, resulting in subsequent corneal injury and opacification, which ultimately required penetrating keratoplasty to restore vision 5 years post injury. A similar case were silver nitrate was used to achieve haemostasis following chalazion removal, resulting in corneal injury was also described by Stein et al., in 1987.2
5. Conclusion with learning points
The authors would suggest storing silver nitrate sticks away from cotton buds with appropriate labelling in order to minimize the risk of inadvertently using a silver nitrate stick to remove a corneal foreign body. It would also be advisable to keep silver nitrate sticks in original packaging and discarding of any unused sticks after a pack has been opened.3 These safety measures are most relevant to A&E departments, as this is likely the highest risk location for such errors to occur as in our case.
- • Silver nitrate sticks can be mistaken for cotton buds
- • Silver nitrate sticks can cause significant corneal injury
- • Storage of silver nitrate sticks away from cotton buds, or in secure locations reduces the risk of error
- • Store silver nitrate sticks in original package and discard unused or remaining silver nitrate sticks after use.
Patient consent
Patient has provided written informed consent.
Funding
No funding or grant support.
Conflicts of interest
The following authors have no financial disclosures: MF, SN, MM, DL.
Authorship
All authors attest that they meet the current ICMJE criteria for Authorship.
Credit author statement
Mustafa Franka: Writing – Original Draft, Writing – Review & Editing, Project administration. Siddarth Nardeosingh: Writing – Review & Editing. Mary-Therese Monaghan: Writing – Review & Editing. Douglas Lyall: Conceptualization, Supervision.
Declaration of competing interest
None.
Acknowledgements
None.
References
Content retrieved from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7900634/.