Forequarter Replantation
An 18-year-old man presented with a workplace-related injury, wherein his left shirt sleeve was caught in a cloth rolling machine and consequently his left upper limb was avulsed and amputated at his shoulder. He presented to our center 3 hours after the incident, with the amputated part brought without cooling. Initial examination showed pallor but no major systemic injuries. The stump site showed exposed upper lateral chest wall without the scapula, with visible axillary vessels and brachial plexus remnants deep in the stump.
The limb was preserved on ice and examined without flushing any fluids. The glenohumeral joint was intact, and attached scapular musculature was avulsed and torn. Distal to the shoulder, there were no bony injuries, as confirmed by radiographs, and no major soft-tissue injuries (Fig.1). After proper counseling, it was decided to attempt a replantation.
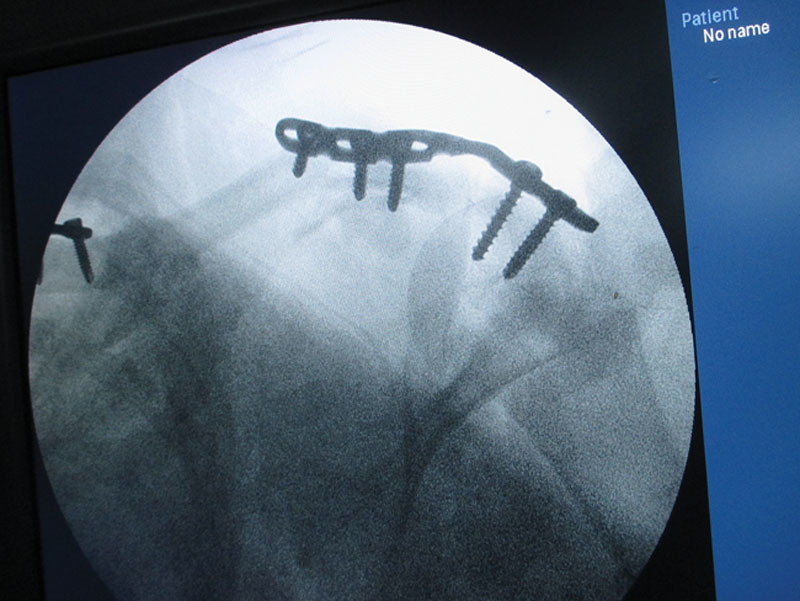
After initial resuscitation, the patient was urgently shifted to the operating room. Thorough debridement of avulsed musculature was done. The axillary artery and vein and the cephalic vein were identified for viable anastomoses. A long-segment vein graft was harvested from the left lower limb. We performed an expedient plating of the acromioclavicular joint, with a view to fixing the scapula to the posterior chest wall at a later date (Fig.2). The anastomoses were then completed, at which time segmental axillary artery loss was noted, which was bridged with the vein grafts (Fig.3).
The brachial plexus elements were found to be avulsed very proximally deep in the stump; hence, primary nerve repair was deemed unadvisable. Revascularization was accomplished at 8 hours post injury (warm ischemia time of 3 hours, cold ischemia time of 5 hours), with good perfusion. Fasciotomies were done in the arm and the forearm. A strong musculotendinous repair was done around the axilla, and the limb strapped to the chest wall.
Postoperatively, the limb was well vascularized as determined by pulse oximetry, clinical examination, and capillary refill. Reperfusion injury, though anticipated, was not seen (normal creatinine, creatine kinase, and blood gas levels). The shoulder musculature showed necrosis after a few days. The patient was taken for serial debridement of unhealthy muscle for a total of 3 sittings (on perioperative antibiotics for 10 days) (Fig.4). Ten days postoperatively, the limb appeared to be infected, though still perfusing.
Higher antibiotics were initiated, and another thorough debridement was done. On day 14, the patient was found to be in sepsis, and his limb was found to be grossly swollen and edematous. Patient was taken for an urgent disarticulation at which time venous thrombosis was noted on table. The stump was closed primarily, and the patient eventually recovered fully and was discharged.

Fig. 4.
Postoperative muscle necrosis.
Author information
From the Department of Plastic Surgery, St. Johns Medical College, Bangalore, Karnataka, India.
Corresponding author.
Aniketh Venkataram, MS (MCh), Department of Plastic Surgery, St. Johns Medical College, 3437, 1st G Cross, 7th Main, Subbanna Gardens Vijaynagar, Bangalore 40, Karnataka, India, E-mail: moc.liamg@vhtekina
References
1. Malt RA, McKhann C. Replantation of severed arms. JAMA. 1964;189:716–722. [PubMed] [Google Scholar]
2. Sabapathy SR, Venkatramani H, Bharathi RR, et al. Technical considerations and functional outcome of 22 major replantations (The BSSH Douglas Lamb Lecture, 2005). J Hand Surg Eur Vol. 2007;32:488–501. [PubMed] [Google Scholar]3. Leclère FM, Mathys L, Juon B, et al. Macroreplantations of the upper extremity: a series of 11 patients. Arch Orthop Trauma Surg. 2012;132:1797–1805. [PubMed] [Google Scholar]4. Larson JV, Kung TA, Cederna PS, et al. Clinical factors associated with replantation after traumatic major upper extremity amputation. Plast Reconstr Surg. 2013;132:911–919. [PubMed] [Google Scholar]
5. Chuang DC, Lai JB, Cheng SL, et al. Traction avulsion amputation of the major upper limb: a proposed new classification, guidelines for acute management, and strategies for secondary reconstruction. Plast Reconstr Surg. 2001;108:1624–1638. [PubMed] [Google Scholar]
6. Laing TA, Cassell O, O’Donovan D, et al. Long term functional results from major limb replantations. J Plast Reconstr Aesthet Surg. 2012;65:931–934. [PubMed] [Google Scholar]
7. Graham B, Adkins P, Tsai TM, et al. Major replantation versus revision amputation and prosthetic fitting in the upper extremity: a late functional outcomes study. J Hand Surg Am. 1998;23:783–791. [PubMed] [Google Scholar]
8. Van Tongel A, Atoun E, Narvani A, et al. Medium to long-term outcome of thoracoscapular arthrodesis with screw fixation for facioscapulohumeral muscular dystrophy. J Bone Joint Surg Am. 2013;95:1404–1408. [PubMed] [Google Scholar]
9. Fufa D, Lin CH, Lin YT, et al. Secondary reconstructive surgery following major upper extremity replantation. Plast Reconstr Surg. 2014;134:713–720. [PubMed] [Google Scholar]10. Cavadas PC. Salvage of replanted upper extremities with major soft-tissue complications. J Plast Reconstr Aesthet Surg. 2007;60:769–775. [PubMed] [Google Scholar]