Impalement head injury with serrated meat knife.
Abstract
An unsuspecting motorcycle passenger was ambushed and impaled on the right side of the head with a 30cm serrated meat carving knife during a sectarian crisis in the city of Jos, Plateau State, Nigeria. The patient escaped running with the knife in his head and was rescued to a military hospital from where he was promptly transferred within 90 minutes of the incident to the Emergency Department of Jos University Teaching Hospital (JUTH), Jos. Prompt resuscitation and CT brain imaging facilitated a successful neurosurgical intervention and a good outcome in the management of this patient.
Introduction
Recurrent sectarian divide has racked Jos, Plateau State of Nigeria in the past eleven years. Hundreds of lives have been lost and serious damage to property and the economy has occurred. Explosive devices, grenades, guns – hand guns, pistols, dane guns, rifles and submachine guns – as well as bombs and suicide bombing have been used. Fires, stones, broken bottles, axes, arrows, spears, machetes and knives make up a list of weapons that have been used to inflict maximum damage and pain as well as serve as an intimidating factor on opponents. The serrated edged meat carving knife that was used on this patient is particularly intimidating and menacing in appearance to the masses and is meant to cut like a saw, shred and tear as well as kill.
The patient, naval rating, part of the peace keeping force in Jos, was off duty and in mufti, had hired a ride as a passenger on a motorcycle. The driver diverted and delivered the passenger to a mob hideout where he was stabbed in an ambush with a 30cm long serrated meat carving knife. He wrestled free and ran away bleeding with the knife in the right side of his head from his assailants to safety where passers-by rushed him to a check point nearby manned by military personnel. There, he lost consciousness and was rushed with the knife still stuck to his head to a military hospital from where he was resuscitated and transferred to the Emergency Department of JUTH, within 90minutes of the incident. He recovered consciousness in JUTH and was able to narrate the incident en route to the operating theatre.
Reports
Presentation
A fully conscious patient in pain with a large knife in his head was able to give a description of what happened to him. He was calm, oriented in time, person and place. He had stable vital signs and was breathing spontaneously. Pulse rate 99 bpm; BP 130/70mm Hg; respiration rate 22/min.
A large serrated edged meat carving knife, 30cm long, covered with blood was jutting out of the right side of the head of the patient as shown in Fig. 1. About 20cm of the knife was visible while the rest was buried about 2.5cm posterior to the right lateral orbital wall and 1cm above the right zygoma. It was directed downwards about 45 degrees to the horizontal and medially by about 30 degrees. He had associated right peri-orbital oedema and subconjunctival haemorrhage. The right pupil was 4mm, sluggishly reacting to light while the left pupil was 2.5mm briskly reactive to light. The other systems were essentially normal. His Haemoglobin and electrolytes were normal.
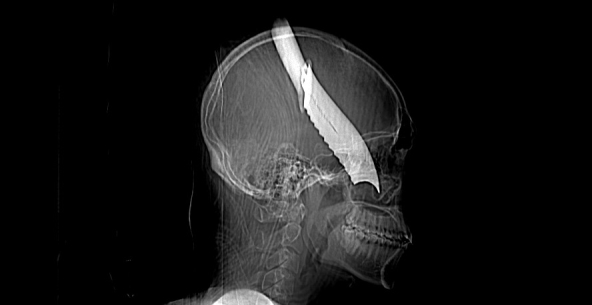
The initial management of the patient was with intravenous saline 100 ml/hr; Ceftriazone 1 gram 12hrly; Metronidazole 500mg 8hrly; intramuscular Diclofenac 75mg 12 hrlyand tetanus toxoid 0.5ml stat. He was nursed 30 degrees head up. Three units of blood were cross-matched for him in preparation for surgery. An urgent CT brain scan showed the trajectory of the knife in his head as shown in Fig. 2. The neurosurgery operating theatre set up was activated with the anaesthetists and the operating nursing staff within an hour of presentation for the exploration and safe retrieval of the knife from the patient’s head.
Pre-operative considerations and objective of neurosurgical intervention
This patient had a knife in his head and the trajectory revealed by CT brain scan did not show the extent of damage to various essential parts of the brain and cranial exploration was the only way to ascertain this. The tamponade effect in the head with the blood vessels as well as severe brain swelling and subsequent increase in intra-cranial pressure had to be taken into consideration in the neurosurgical approach and exposure of the brain in this patient. Extra cranial carotid ligations to effect vascular control, frontal lobectomy as well as decompressive hemicraniectomy were also prepared for.
The objectives of neurosurgical intervention in this patient were the safe and complete removal of the knife with minimal intra-operative complications, secure haemostasis and achieve debridement.
Surgical Technique
In the operating theatre, patient in the supine position was intubated and put under general anaesthesia. The right side of the head was positioned uppermost for access in a Mayfield head clamp. Routine cleansing with savlon and iodine and draping for a right temporo-frontal craniotomy as well as carotid access was done. A right temporo-frontal scalp incision incorporating the stab wound as the anterior end of the incision was made. A right temporo-frontal craniotomy incorporating the knife was raised to visualize the area. This showed intact dura and the trajectory of the knife as entirely extra-cranial into the right maxillary air sinus. The knife was gently manipulated in the anterior-posterior and lateral axes till it was free to be delivered from the wound. There was no gush of blood at inspection although there was bleeding from the bone edges. Haemostasis was secured with bone wax. The wound was irrigated copiously with normal saline and hydrogen peroxide and a drain left in situ. The bone flap was replaced and secured with 2/0 vicryl, the scalp closed in two layers and silk to skin.
Post operative period
The immediate post operative period was smooth and he had an uneventful recovery from anaesthesia. He was continued on intravenous antibiotics for another 5 days. The drain was removed after 24hrs. The patient made an uneventful recovery as shown in Fig. 3. He was discharged home after 2 weeks of admission, fully recovered and had had no neurological deficit six months after the surgery.
Serrated edged meat-carving knife impaled in the right fronto-temporal region of the patient
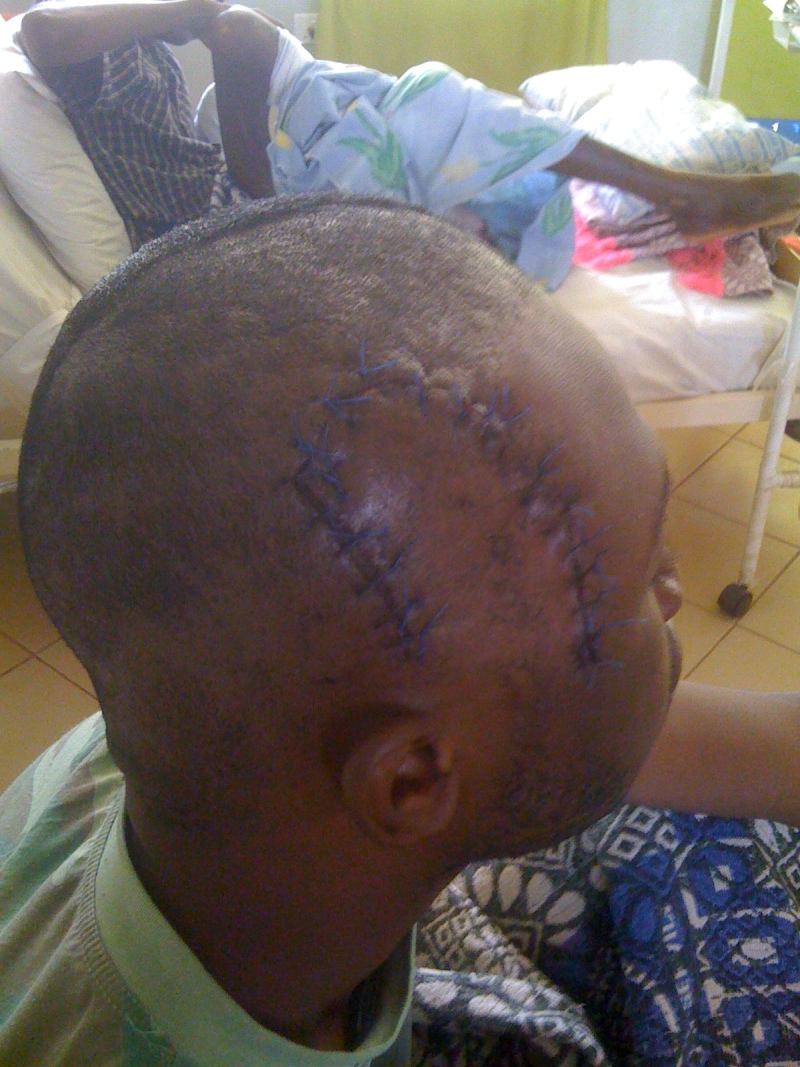
Patient without the large serrated meat knife
References
References
1. Penetrating Craniofacial Injury in a Pediatric Patient. Journal of Craniofacial Surgery. 2012;13(2):303–307. [Abstract] [Google Scholar]2. Michael DB. Gunshot wounds to the head. Contemp Neurosurg . 1995;17:15–15. [Google Scholar]3. Taphonomy – Edged, Incised, Hacking, and Impaling Traumas. Taphonomy – Edged, Incised, Hacking, and Impaling Traumas. http://www.mercyhurst edu/ files/applied-forensic-sciences/2011taphonomy-trauma 493http://www.mercyhurst edu/ files/applied-forensic-sciences/2011taphonomy-trauma 4934. Eppley BL. Craniofacial impalement injury: a rake in the face. J Craniofac Surg. 2002;13:35–7. [Abstract] [Google Scholar]5. Sasser SM, Hunt RC, Sullivent EE. Recommendations of the National Expert Panel on Field Triage. RR-1. Vol. 58. MMWR Recomm Rep 2009; 2009. Guidelines for field triage of injured patients; pp. 1–35. [Abstract] [Google Scholar]6. Kjelland C, Thirsk W. Penetrating craniofacial trauma from a vice clamp: case report and discussion. CJEM. 2011;13(1):57–61. [Abstract] [Google Scholar]7. Youssef AS, Morgan JM, Padhya T. Penetrating craniofacial injury inflicted by a knife. J Trauma. 2008;64:1622–24. [Abstract] [Google Scholar]8. Kaye K, Kilgore KP, Grorud C. Transoral crossbow injury: an unusual case of central nervous system foreign body. J Trauma. 2004;57:653–5. [Abstract] [Google Scholar]
Articles from Journal of the West African College of Surgeons are provided here courtesy of West African College of Surgeons
Copyright and License
Copyright © 2012, THe West African College of Surgeons
Original Source
Changes from original article
“Conclusions” and “Discussion” have been removed from the original article to make the article a little shorter.