Case report of Wolfe grafting for the management of bilateral cicatricial eyelid ectropion following severe burn injuries
Case Report
31-year-old Caucasian man was referred for treatment at our institution for surgical treatment of the cicatricial ectropion of both lower eyelids and exposure keratopathy due to severe deep dermal burns that affected minimally 60% of the TBSA (Fig. 1).

Cicatricial ectropion in both lower eyelids, left eye more affected, before the surgery.
Eight months prior to this presentation, patient sustained thermal burn injuries. Mechanism of the injury was explained by patient as being doused with large amount of gasoline and set ablaze in closed space. Initial diagnosis stated that head, face, neck, breast, lower and upper bilateral extremities were affected with deep dermal and third-degree burns; urinary fistula; sepsis; paresis of the peronei nerve on the right side; both lids contractures; contractures and deformities of the both hands fingers. Primary treatment was obtained at the largest hospital in the country due the need for mechanic ventilation and intensive reanimation therapy. All burns were covered with bandages. Patient received decompressive fasciotomy and was transferred to subspecialized university clinic in other country (out-country treatment) for prolonged medical treatment that lasted seven months. There, he received 13 surgeries: several necrotomies and the Meek Micrografting technique procedures with two repeated keratinocytes cultures harvesting in their tissue bank. Due to prolonged respiratory treatment, a tracheostomy was performed. Patient had multiple times sepsis and bacterial cultures showed mixed gram positive and negative resistant organisms; therefore, often change of antibiotics’ regime was applied. After multiple surgical treatments, lids, earlobe and fingers were still left with deformities. The patient was released from aforementioned institution in good general condition and recommendation for in-home-country surgical treatment of the lids.
Patient was referred to our hospital for the continuation of conservative treatment and lid surgeries. Here, we isolated following microbes during bacterial cultivations: Coagulase negative staphylococcus, Proteus Mirabilis, Staphylococcus aureus, Pseudomonas Aeruginosa and Species, and appropriate antibiotic treatment was given. Our examination found: multiple non-epithelized body areas (1–3 cm surface on average), damaged periocular and lid skin with scaring, cicatricial ectropion of both lower eyelids, complete loss of eye brown, upper lids with decreased motility, eyelashes somewhat preserved, eye ball fine, conjunctival hyperemia, right cornea with macula in the optic zone, left cornea with superficial 6 o’clock erosion. Best corrected visual acuity on the right eye was 7/200 and on the left eye 20/20, examined using standard Snellen eye chard from the distant of 6 m, with normal eye pressure. Plastic surgeons and ophthalmologists performed bilateral lower eyelids reconstructive surgery at the department of plastic and reconstructive surgery in the general endotracheal anesthesia. Surgical protocol was as follows: patient’s surgical site antiseptic skin preparation with aqueous iodine (10%), followed by right and subsequently left lower eyelid skin incision and excision of cicatricial tissue 5 mm below the cilia from canthus-to-canthus with orbicularis presentation. Scaring tissue was excised, and tissue above orbicularis was bluntly dissected, aiming to release contracture and elevate the lid. This produced left lower eyelid with excess tissue including both lamellas, accompanied with severe posterior lamella medially located focal damage; therefore, we made full thickness pentagonal wedge excision on the left lower eyelid of approximately 20% of the total lid surface. The defect was sutured using mattress suture technique. A wound bed in a size of 20 × 15mm right, and 25 × 20 mm on the left side remained in lower eyelids. Due to extensive skin damage and scaring tissue after auto-transplantation along the entire body surface, we used only available and suitable healthy skin for grafting method from the left inner upper thigh (inguinal region). The left inguinal surgical site region was preoperatively prepared and cleaned with aqueous iodine (10%), and the full-thickness skin graft was taken (Wolfe technique), to replace the skin defect on the both lower eyelids. Graft was sutured using the 6.0 non-absorbable nylon suture and secured with tie-over tamponade on the both sides (Fig. 2). First inspection was made 72 hours after; tamponade was released, and the wound treated. Graft was 100% viable and of appropriate colour. Two days after, all dressing was taken off, graft exposed, and no additional dressing was applied on the both sides. On the third postoperative day, lid positions were satisfying, no corneal exposure was marked, good lid motility was obtained and preserved on the both sides, 6 months follow up grafts had good colour with no signs of necrosis, or discoloration, only showing mild medial ectropion on the left lower lid, but with no extensive corneal exposure (Fig. 3).

Fig. 2. Sensitive image, click to unblur
Wolfe full-thickness skin graft on both eyelids during the surgery. Graft was sutured using the 6.0 non-absorbable nylon suture (left eye), and secured with tie-over tamponade (right eye).
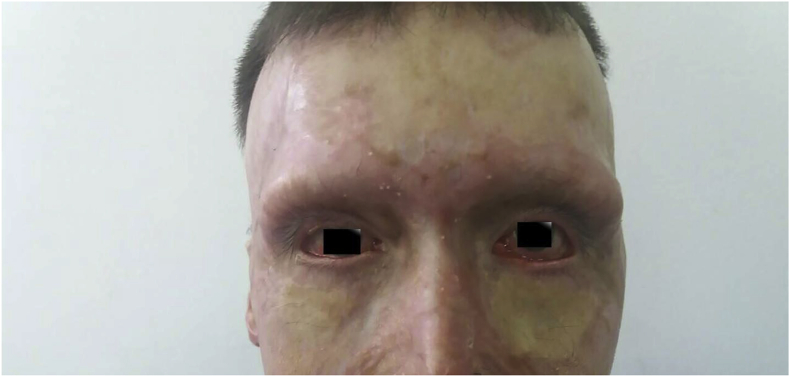
Patient 6 months after the surgery; grafts had good colour with no signs of necrosis, or discoloration, only showing mild medial ectropion on the left lower lid, but with no extensive corneal exposure.
Author
∗Corresponding author: Ophthalmology Department, Canton Hospital Zenica, Str. Crkvice 67, 72000 Zenica, Bosnia and Herzegovina.
Nina Jovanovic, Admira Dizdarevic, Nedzad Dizdarevic, Amir Haracic, Lamija Gafurovic.